I. Preoperative Assessment
A thorough evaluation is crucial, encompassing risk stratification, detailed medical history, and a focused cardiac physical exam.
Electrocardiograms and biomarkers (Troponin, BNP) aid in identifying potential risks before surgery.
Risk Stratification
Effective risk stratification is the cornerstone of perioperative cardiac care, particularly when patients undergo noncardiac surgery. A careful clinical evaluation aims to predict the likelihood of adverse cardiovascular events, guiding decisions about surgical postponement, optimization, or proceeding with caution.
Several validated risk indices, such as the Revised Cardiac Risk Index (RCRI), assist in categorizing patients based on factors like history of heart failure, recent myocardial infarction, cerebrovascular disease, diabetes mellitus, chronic kidney disease, and the severity of the planned surgical procedure.
Recognizing that up to 50% of perioperative myocardial infarctions may be unrecognized underscores the importance of a high index of suspicion. Guidelines from the ACC/AHA emphasize a stepwise approach, tailoring the intensity of evaluation to the patient’s risk profile and the invasiveness of the surgery. This process ensures appropriate resource allocation and individualized care plans.
Comprehensive Medical History
A detailed medical history is paramount in assessing perioperative cardiac risk. This includes a thorough review of pre-existing cardiovascular conditions – coronary artery disease, heart failure, valvular heart disease, and arrhythmias – along with their severity and current management.
Specifically, document prior myocardial infarctions, percutaneous coronary interventions (PCI), or coronary artery bypass grafting (CABG). Inquire about symptoms of angina, dyspnea, or lower extremity edema. A complete medication list is essential, noting antiplatelet agents, anticoagulants, beta-blockers, and any cardiac-specific medications.
Beyond cardiac history, gather information on hypertension, diabetes mellitus, renal insufficiency, and pulmonary disease, as these comorbidities significantly impact perioperative risk. Understanding the patient’s functional capacity – their ability to perform activities of daily living – provides valuable insight into their overall cardiovascular reserve. This comprehensive approach informs subsequent evaluation and optimization strategies.
Physical Examination Focused on Cardiac Status
The cardiac-focused physical exam aims to identify signs of underlying cardiovascular disease and assess its severity. Begin with vital sign assessment, noting blood pressure, heart rate, and respiratory rate. Auscultate the heart for murmurs, gallops, or rubs, carefully characterizing their timing and location.
Evaluate for jugular venous distension (JVD) and peripheral edema, indicators of potential heart failure. Palpate peripheral pulses to assess for peripheral artery disease. Assess for signs of hypoperfusion, such as cool extremities or delayed capillary refill.
Lung auscultation is crucial to detect crackles or wheezes suggestive of pulmonary congestion. A thorough examination should also include assessment of the carotid arteries for bruits. Document any limitations to exercise tolerance. These findings, combined with the medical history and other investigations, contribute to a comprehensive perioperative risk assessment.
Electrocardiogram (ECG) Interpretation
A 12-lead ECG is fundamental in the preoperative assessment, providing insights into cardiac rhythm, rate, and evidence of ischemia, infarction, or left ventricular hypertrophy. Look for signs of prior myocardial infarction – Q waves, T-wave inversions, or ST-segment abnormalities. Assess for arrhythmias, including atrial fibrillation or bradycardia, which may require specific management.
Evaluate the QT interval, as prolonged QT can increase the risk of torsades de pointes. Identify bundle branch blocks or other conduction abnormalities. Pay attention to signs of left ventricular hypertrophy, such as increased R-wave voltage in the left ventricular leads.
Compare the current ECG to any prior tracings to identify new changes. ECG findings should be correlated with the patient’s clinical presentation and cardiac biomarkers. A normal ECG does not exclude underlying cardiac disease, but abnormal findings necessitate further investigation and optimization before surgery.
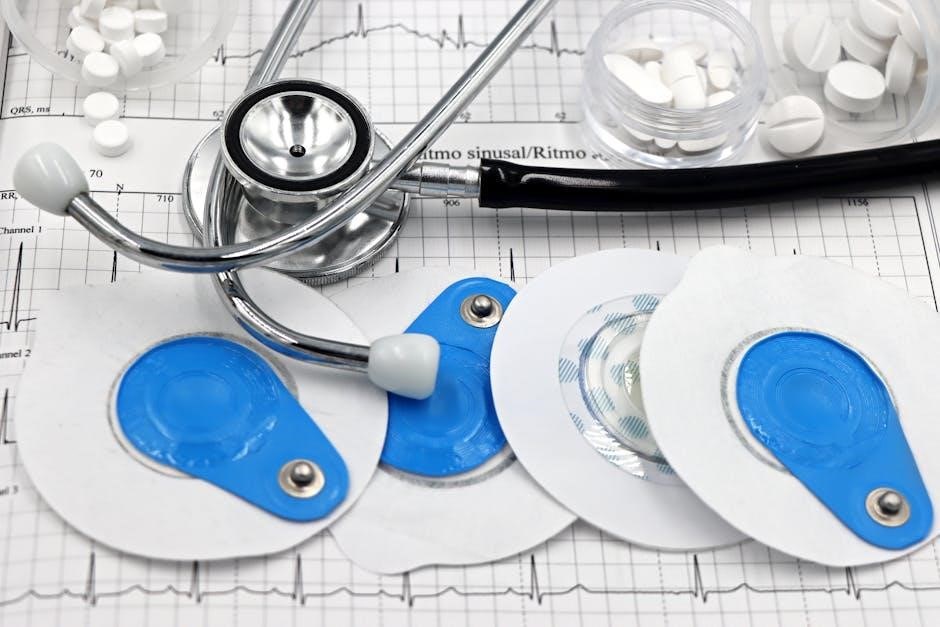
Cardiac Biomarkers (Troponin, BNP)
Cardiac biomarkers offer crucial objective data to assess myocardial injury and heart failure risk. Troponin I or T levels should be measured, as elevated levels indicate myocardial necrosis, even in the absence of classic ischemic symptoms. A rise and/or fall in troponin values suggests perioperative myocardial infarction (MI).
B-type natriuretic peptide (BNP) or N-terminal pro-BNP (NT-proBNP) levels are valuable in evaluating the risk of heart failure and predicting adverse cardiovascular events. Elevated BNP suggests increased ventricular wall stress and may indicate underlying cardiac dysfunction.
Serial biomarker measurements may be necessary, particularly in high-risk patients. Interpretation requires clinical context; elevated biomarkers don’t always equate to actionable intervention but inform risk stratification. These tests help guide decisions regarding surgical postponement or optimization.
II. Preoperative Optimization
Optimizing cardiac status is key, focusing on blood pressure, diabetes, and lipid control. Careful management of anticoagulants and beta-blockers is essential for positive outcomes.
Management of Hypertension
Hypertension requires careful preoperative assessment and optimization. Continuation of existing antihypertensive medications is generally recommended, with adjustments made based on individual patient factors and the specific surgical procedure. Avoid abrupt discontinuation, as this can lead to rebound hypertension or withdrawal syndromes.
For patients with poorly controlled hypertension, delaying elective surgery may be considered until blood pressure is adequately managed. Intraoperative blood pressure control is paramount, utilizing short-acting agents for rapid adjustments. Beta-blockers can be particularly useful in managing hypertension and controlling heart rate during surgery, especially in patients with coronary artery disease.
Postoperatively, close monitoring of blood pressure is essential, with prompt treatment of both hypertension and hypotension. ERAS protocols emphasize proactive pain management, as uncontrolled pain can contribute to hypertension. A stepwise approach, starting with non-pharmacological interventions and escalating to medications as needed, is generally preferred. Individualized blood pressure targets should be established based on the patient’s pre-operative status and overall health.
Control of Diabetes Mellitus
Optimal glycemic control is vital in diabetic patients undergoing cardiac surgery, minimizing risks of infection, wound healing complications, and cardiovascular events. Preoperative assessment should include HbA1c levels to gauge long-term control. Avoid significant fluctuations in blood glucose around the time of surgery.
Continue most oral hypoglycemic agents up to the day of surgery, except for metformin, which should be held 24-48 hours prior to reduce lactic acidosis risk. Insulin regimens require careful adjustment, often transitioning to a basal-bolus approach for tighter control. Intraoperative glucose monitoring every 1-2 hours is crucial, with insulin infusions used to maintain target levels (typically 140-180 mg/dL).
Postoperative glucose management should continue with frequent monitoring and insulin adjustments. ERAS protocols support early oral feeding to facilitate glucose control. Proactive management of hyperglycemia and hypoglycemia is essential for optimal recovery and reduced morbidity. Close collaboration between the surgical and endocrinology teams is highly recommended.
Lipid Management & Statin Therapy
Statins play a crucial role in perioperative cardiac care, demonstrating benefits in reducing myocardial infarction, stroke, and mortality, even in patients without pre-existing statin use. Continue statin therapy throughout the perioperative period unless contraindicated. Abrupt discontinuation can lead to adverse outcomes.
For patients not already on statins, consider initiating high-intensity statin therapy prior to surgery, particularly those with established cardiovascular disease or multiple risk factors. Meta-analyses support perioperative statin use, showing significant reductions in complications. Monitor lipid levels postoperatively to assess treatment effectiveness.
Address other lipid abnormalities as indicated, but statins remain the cornerstone of lipid management. ERAS protocols integrate statin continuation into the overall care pathway. Careful consideration should be given to potential drug interactions and renal function when prescribing statins. Proactive lipid management contributes to improved long-term cardiovascular health.
Antiplatelet and Anticoagulation Management
Managing antiplatelet and anticoagulant medications is paramount to balance bleeding risk and thromboembolic events. Develop a clear plan for each patient based on the specific agent, indication, and surgical procedure. Guidelines recommend holding agents with significant bleeding risks prior to surgery.
For patients on dual antiplatelet therapy (DAPT) after stent placement, the duration of interruption should be individualized. Consider the stent type (DES vs. BMS) and the risk of stent thrombosis. Anticoagulants, such as warfarin or direct oral anticoagulants (DOACs), require careful bridging strategies if interruption is necessary.
Minimize the interruption period whenever possible, and resume medications postoperatively as soon as hemostasis is assured. Close communication between the surgical, cardiology, and anesthesia teams is essential. Document the plan clearly in the patient’s record. Perioperative management of these medications significantly impacts patient safety.
Beta-Blocker Therapy Considerations
Perioperative beta-blocker management requires careful consideration, particularly in patients with coronary artery disease or heart failure. Abrupt discontinuation can lead to rebound hypertension, tachycardia, and increased myocardial oxygen demand, potentially precipitating cardiac events. Current guidelines generally recommend continuing beta-blocker therapy throughout the perioperative period.
However, individualize the approach based on the patient’s clinical status and the nature of the surgery. For patients undergoing non-cardiac surgery, continue beta-blockers if they were previously on them. If a patient is not already on a beta-blocker, initiation solely for perioperative stress reduction is generally not recommended.
Monitor hemodynamics closely and adjust beta-blocker dosage as needed. Be prepared to manage hypotension or bradycardia. The ACC and AHA have emphasized beta-blocker therapy as a quality measure in evidence-based care, highlighting its importance in optimizing outcomes.
III. Intraoperative Management
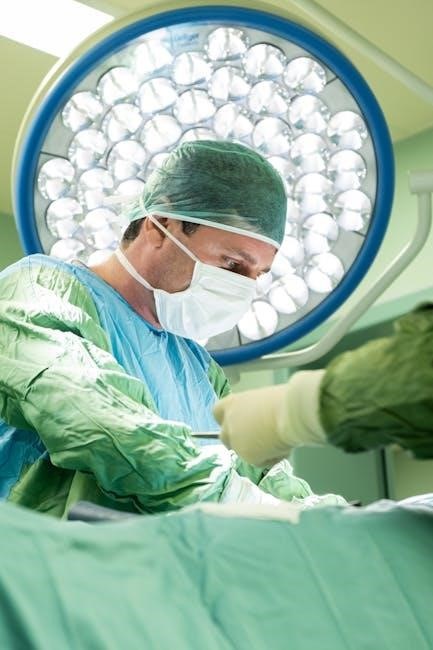
Anesthetic choices and monitoring are vital for cardiac patients. Hemodynamic stability, arrhythmia management, and myocardial protection strategies are key. TEE provides real-time cardiac function assessment.
Anesthetic Considerations for Cardiac Patients
Anesthetic selection significantly impacts cardiac patients undergoing surgery. Maintaining hemodynamic stability is paramount, often requiring careful titration of vasoactive medications and fluid management. Volatile anesthetics, while offering advantages, can depress myocardial function and induce arrhythmias, necessitating vigilant monitoring. Total intravenous anesthesia (TIVA), utilizing propofol and opioids, provides greater hemodynamic control but demands meticulous titration to avoid hypotension.
Regional anesthesia techniques, when feasible, can minimize systemic effects and sympathetic activation. Neuromuscular blocking agents should be used judiciously, considering their potential to exacerbate cardiac dysfunction. Attention to temperature regulation is crucial, as hypothermia can increase the risk of arrhythmias and myocardial ischemia. Preemptive analgesia, utilizing multimodal approaches, minimizes postoperative pain and sympathetic stress. Close communication between the anesthesiologist, surgeon, and cardiologist is essential for optimizing anesthetic management and mitigating cardiac risks.
Hemodynamic Monitoring
Robust hemodynamic monitoring is vital for cardiac surgical patients, guiding fluid and vasopressor management. Arterial blood pressure monitoring provides continuous, real-time data, enabling prompt identification of hypotension or hypertension. Central venous pressure (CVP) assessment aids in evaluating right atrial pressure and fluid status, though its interpretation requires caution. Pulmonary artery catheters (PACs), while less commonly used, offer comprehensive hemodynamic data, including pulmonary artery pressures and cardiac output.
Non-invasive monitoring, such as echocardiography (TEE), provides valuable information on ventricular function, valve competence, and preload. Stroke volume variation (SVV) and pulse pressure variation (PPV), derived from arterial waveform analysis, can assess fluid responsiveness in mechanically ventilated patients. Continuous ECG monitoring is essential for detecting arrhythmias and ischemic changes. Regular assessment of urine output serves as a marker of renal perfusion and overall hemodynamic status. Integrating data from multiple monitoring modalities allows for a comprehensive understanding of the patient’s hemodynamic state.
Management of Arrhythmias
Perioperative arrhythmias are common following cardiac surgery, requiring prompt recognition and management. Atrial fibrillation (AF) is particularly prevalent, often treated with rate control using beta-blockers or calcium channel blockers. Antiarrhythmic drugs, such as amiodarone, may be considered for rhythm control, but carry potential side effects. Bradycardia necessitates assessment for underlying causes, potentially requiring temporary pacing.
Ventricular arrhythmias, though less frequent, demand immediate attention, potentially involving defibrillation or antiarrhythmic medications like lidocaine. Continuous ECG monitoring is crucial for early detection. Electrolyte imbalances (potassium, magnesium) should be corrected promptly, as they can trigger arrhythmias. Hypoxia and ischemia must be addressed aggressively. Transesophageal echocardiography (TEE) can help identify structural heart disease contributing to arrhythmias. A systematic approach, guided by ACLS protocols, is essential for effective arrhythmia management.
Myocardial Protection Strategies
Protecting the myocardium during cardiac surgery is paramount. Cardioplegia, inducing cardiac arrest with a specialized solution, remains a cornerstone technique, minimizing ischemic damage. Intermittent cardioplegia, with repeated infusions, is often preferred over continuous delivery. Hypothermic circulatory arrest can be employed for complex procedures, further reducing metabolic demand.
Pharmacological interventions, such as administration of antioxidants and remote ischemic preconditioning, are explored to enhance myocardial resilience. Minimizing aortic cross-clamp time is crucial, achieved through meticulous surgical technique and efficient workflow. Maintaining adequate perfusion pressure during cardiopulmonary bypass is vital. Transesophageal echocardiography (TEE) guides assessment of myocardial function and identifies regional wall motion abnormalities. Postoperative monitoring for evidence of myocardial injury, via cardiac biomarkers, is essential to evaluate the effectiveness of these protective strategies.
Transesophageal Echocardiography (TEE)
Transesophageal echocardiography (TEE) is an indispensable tool in perioperative cardiac care, offering superior imaging compared to transthoracic echocardiography. Real-time visualization of cardiac structures allows for assessment of ventricular function, valve morphology, and the presence of intracardiac thrombi. During surgery, TEE guides cannulation, monitors regional wall motion, and detects air emboli or complications like valve dehiscence.
TEE aids in evaluating hemodynamic status, assessing volume responsiveness, and guiding fluid management. Its use extends to identifying and managing arrhythmias, and evaluating the effectiveness of myocardial protection strategies. Postoperatively, TEE detects pericardial effusion, assesses ventricular filling pressures, and monitors for postoperative complications. Experienced sonographers and cardiologists are crucial for optimal image acquisition and interpretation, ensuring informed clinical decision-making throughout the perioperative period.
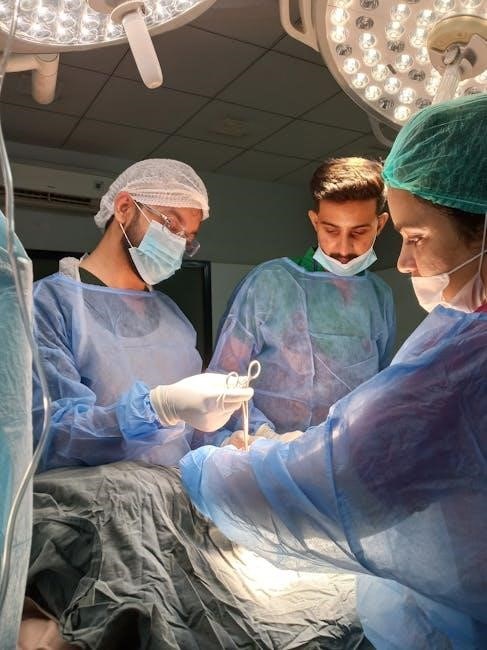
IV. Postoperative Care
Intensive monitoring in the ICU is vital, alongside tailored pain management and strategies to prevent atrial fibrillation. Promptly address potential complications like MI or stroke, utilizing ERAS protocols for recovery.
Early Postoperative Monitoring (ICU)
Immediate postoperative care within the Intensive Care Unit (ICU) is paramount for cardiac surgery patients. Continuous electrocardiographic monitoring is essential to detect arrhythmias, including atrial fibrillation, which is a common post-operative occurrence. Arterial blood pressure monitoring, utilizing an arterial line, allows for precise hemodynamic assessment and titration of vasoactive medications.
Central venous pressure (CVP) monitoring aids in evaluating fluid status and optimizing cardiac output. Frequent assessment of oxygen saturation via pulse oximetry, alongside arterial blood gas analysis, ensures adequate tissue perfusion. Serial cardiac biomarkers, such as troponin, should be monitored to identify potential myocardial injury.
Close attention to urine output serves as an indicator of renal function and overall hemodynamic stability. Chest X-rays are routinely performed to assess for pulmonary complications, like pneumothorax or pulmonary edema. Neurological assessments are crucial to detect any signs of stroke or altered mental status. Pain management protocols, utilizing multimodal analgesia, are implemented to minimize discomfort and promote early mobilization.
Pain Management Protocols
Effective pain control is a cornerstone of postoperative care following cardiac surgery, directly impacting recovery and minimizing complications. Multimodal analgesia is the preferred approach, combining various pharmacological and non-pharmacological techniques. Opioids, while effective, should be used judiciously to minimize respiratory depression and other adverse effects.
Non-opioid analgesics, such as acetaminophen and nonsteroidal anti-inflammatory drugs (NSAIDs – if renal function permits), play a crucial role in reducing opioid consumption. Regional anesthesia techniques, including epidural or paravertebral analgesia, can provide excellent pain relief with minimal systemic effects.
Proactive pain management, rather than reactive, is essential. Regular pain assessments using validated scales are vital to tailor analgesia to individual patient needs. Non-pharmacological interventions, like positioning, relaxation techniques, and early mobilization, complement pharmacological approaches. Enhanced Recovery After Surgery (ERAS) protocols emphasize preemptive analgesia and minimizing pain-related stress responses.
Prevention of Postoperative Atrial Fibrillation
Postoperative atrial fibrillation (POAF) is a common complication following cardiac surgery, increasing the risk of stroke, hemodynamic instability, and prolonged hospital stays. Proactive strategies are crucial for prevention. Beta-blocker therapy, initiated preoperatively and continued postoperatively, remains a cornerstone of POAF prophylaxis, though individualized assessment is key.
Maintaining sinus rhythm through meticulous electrolyte management – particularly potassium and magnesium – is vital. Avoiding hypovolemia and aggressive fluid management can also reduce POAF incidence. Consideration should be given to prophylactic antiarrhythmic agents, such as amiodarone or dronedarone, in high-risk patients, weighing benefits against potential side effects.
Early ambulation and minimizing surgical trauma contribute to POAF prevention. Continuous cardiac monitoring allows for prompt detection and management of arrhythmias; ERAS protocols, emphasizing minimized inflammation and optimized physiological function, indirectly reduce POAF risk.
Management of Postoperative Complications (MI, Stroke)
Prompt recognition and management of postoperative myocardial infarction (MI) and stroke are paramount. Unrecognized MIs are surprisingly common post-surgery, potentially reaching up to 50% of perioperative events. Serial ECGs and cardiac biomarkers (Troponin) are essential for early detection. Treatment mirrors standard MI protocols: oxygen, aspirin, nitroglycerin, morphine, and potential revascularization.
Postoperative stroke requires rapid assessment – differentiating ischemic from hemorrhagic events via CT or MRI. Thrombolytic therapy may be considered within appropriate time windows for ischemic strokes, guided by strict inclusion/exclusion criteria. Blood pressure control is crucial, avoiding both hypotension and excessive hypertension.
Neurological monitoring and close observation in the ICU are vital. ERAS protocols, minimizing inflammation and optimizing hemodynamics, can indirectly reduce the risk of both MI and stroke. Early rehabilitation and multidisciplinary care are essential for optimal recovery and minimizing long-term disability.
Enhanced Recovery After Surgery (ERAS) Protocols
ERAS protocols represent a paradigm shift in postoperative care, aiming to accelerate recovery and reduce complications following cardiac surgery. These evidence-based guidelines, developed by the ERAS Cardiac Society, focus on optimizing patient outcomes through a multidisciplinary approach.
Key components include preoperative counseling, minimizing surgical stress, meticulous hemodynamic management, and multimodal analgesia – reducing opioid reliance. Early mobilization, proactive nutritional support, and strict glycemic control are also central. ERAS protocols emphasize patient engagement and education.
By minimizing the inflammatory response and promoting early return to function, ERAS protocols demonstrably shorten hospital stays, decrease complication rates (including atrial fibrillation), and improve long-term quality of life. Adherence to these protocols is increasingly recognized as a quality measure in cardiac surgical programs.
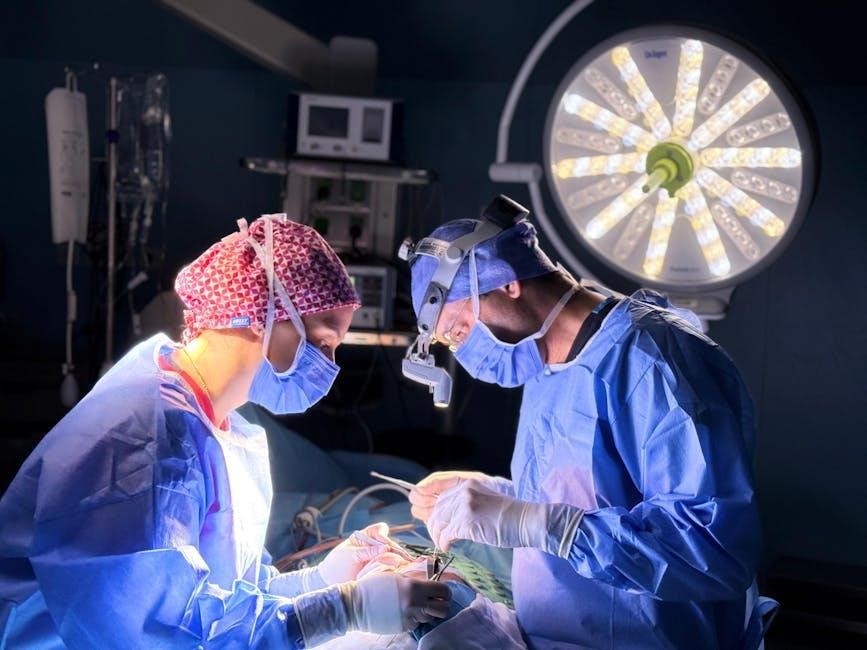
V. Long-Term Follow-Up
Continuous monitoring is essential, including medication reconciliation, cardiac rehabilitation, and lifestyle adjustments. Ongoing risk factor management ensures sustained cardiovascular health post-surgery.
Medication Reconciliation and Adherence
Meticulous medication reconciliation is paramount during long-term follow-up, encompassing a comprehensive review of all prescribed medications – including those initiated preoperatively, adjusted intraoperatively, or newly prescribed postoperatively. This process aims to identify and resolve discrepancies, preventing potentially harmful drug interactions or omissions.
Patient education is key to fostering adherence. Clear, concise explanations regarding medication purpose, dosage, timing, and potential side effects are vital. Utilizing simplified medication schedules and pill organizers can further enhance compliance. Addressing patient concerns and barriers to adherence, such as cost or complexity, is equally important.
Regular follow-up appointments provide opportunities to reinforce medication adherence and assess for any adverse effects. Pharmacists can play a crucial role in this process, offering medication counseling and monitoring. Non-adherence should be addressed with empathy and a collaborative approach, exploring potential solutions to improve patient outcomes and minimize cardiovascular risk.
Documentation of medication lists and adherence strategies within the electronic health record ensures continuity of care across healthcare settings.
Cardiac Rehabilitation
Cardiac rehabilitation (CR) is a cornerstone of long-term recovery following cardiac surgery, significantly improving functional capacity, quality of life, and reducing future cardiovascular events. A comprehensive CR program typically includes supervised exercise training, nutritional counseling, and psychosocial support.
Exercise sessions are tailored to each patient’s individual needs and progress, gradually increasing intensity and duration. Monitoring during exercise is crucial to ensure safety and effectiveness. Nutritional guidance focuses on adopting a heart-healthy diet, managing weight, and controlling cholesterol and blood pressure.
Psychosocial support addresses anxiety, depression, and other emotional challenges often experienced post-surgery. Education on risk factor modification – including smoking cessation and stress management – empowers patients to take control of their health.
Early referral to CR, ideally during hospitalization, maximizes participation rates and long-term benefits. Adherence to the CR program is vital for achieving optimal outcomes and sustained improvements in cardiovascular health.
Lifestyle Modifications
Sustained lifestyle changes are paramount for long-term cardiac health following surgery, complementing medical therapies and enhancing overall well-being. Smoking cessation is critical, dramatically reducing cardiovascular risk and improving surgical outcomes. Patients should be strongly encouraged to quit and provided with resources for support.
Adopting a heart-healthy diet – rich in fruits, vegetables, whole grains, and lean protein – is essential. Limiting saturated and trans fats, cholesterol, sodium, and added sugars is crucial. Regular physical activity, at least 150 minutes of moderate-intensity exercise per week, improves cardiovascular function and helps maintain a healthy weight.
Effective stress management techniques, such as yoga, meditation, or deep breathing exercises, can lower blood pressure and reduce the risk of arrhythmias. Maintaining a healthy weight through diet and exercise reduces strain on the heart.
Regular monitoring of blood pressure, cholesterol, and blood sugar levels is vital, alongside adherence to prescribed medications. These modifications, consistently implemented, contribute significantly to long-term cardiac health.
Ongoing Risk Factor Management
Continuous management of pre-existing risk factors is fundamental to preventing future cardiac events post-surgery. Hypertension control remains vital, requiring regular monitoring and medication adjustments as needed to achieve target blood pressure levels. Diabetes management, including blood glucose monitoring and adherence to dietary recommendations and medications, is equally crucial.
Lipid management, often involving statin therapy, should be maintained to optimize cholesterol levels and reduce atherosclerotic plaque progression. Regular follow-up appointments with a cardiologist are essential for assessing cardiac function and adjusting treatment plans. Addressing obesity through lifestyle modifications or, when appropriate, medical interventions, is also key.
Monitoring for and managing atrial fibrillation, a common post-operative complication, is important. Patient education regarding medication adherence, lifestyle modifications, and recognizing symptoms of cardiac issues is paramount. Proactive intervention and consistent monitoring are vital for long-term cardiac health.
